Relief from Sciatica: How Massage Therapy Can Help (And What's Really Going On Back There)
Let me start with something I hear constantly in my work as a mobile massage therapist in Los Angeles:
"I think it's my sciatica."
And look, I get it. Pain that shoots down your leg, aching through your glutes, weird tingling that makes you shift around in your chair all day — it's miserable, and "sciatica" is the word everyone knows. It's basically become the "carpal tunnel" of lower body pain. Got a twitch in your wrist? Carpal tunnel. Got anything happening from your lower back to your toes? Sciatica.
The truth is a little more complicated. But the good news? Whether it's true sciatica or one of the many conditions that mimic it, massage therapy can genuinely help. Let me explain what's actually going on, and why this is one of my favorite problems to work on.
First: What Is Sciatica, Actually?
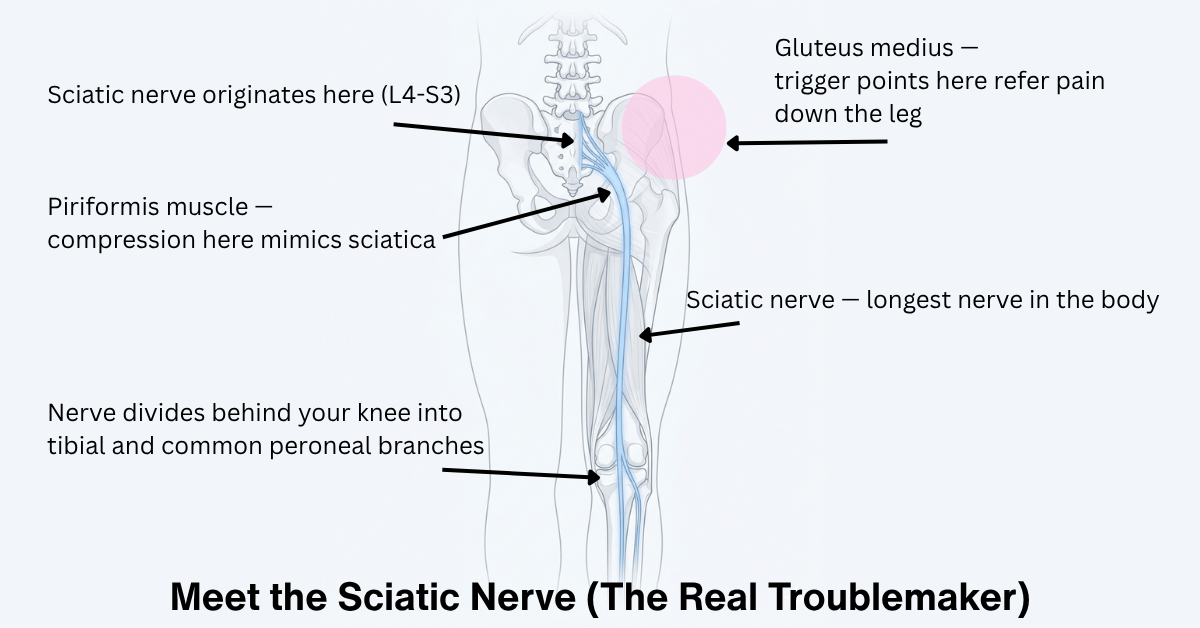
True sciatica is compression or irritation of the sciatic nerve — the longest nerve in the human body, running from your lower spine all the way down through your glutes, hamstrings, calves, and into your feet. When something is pressing on that nerve (a herniated disc, bone spur, or narrowing of the spinal canal), you get the classic symptoms: a sharp, burning, or shooting pain that radiates down one leg, sometimes accompanied by numbness, tingling, or weakness.
Here's the thing though: a lot of what people call "sciatica" isn't actually nerve compression at the spine. It's something else entirely — usually tight muscles putting pressure on the nerve further down the chain. The most common culprit?
The piriformis.
That small but mighty muscle deep in your glute can, when it gets tight or inflamed, press directly on the sciatic nerve as it passes through (or in some people, right through) the muscle. This is called piriformis syndrome, and it produces symptoms that are nearly identical to disc-related sciatica. Same shooting pain. Same leg weirdness. Completely different source.
Other mimics include:
Tight hamstrings pulling on the sit bones and compressing surrounding tissue
Trigger points in the gluteus minimus (which can refer pain all the way down the leg)
SI joint dysfunction
Hip flexor tightness changing the mechanics of the entire lower back and pelvis
I've worked on dozens of clients in Beverly Hills, West Hollywood, Encino, and across the Valley who came to me convinced they had a disc problem — only to find that four or five focused sessions on the glutes, piriformis, and lumbar region made a dramatic difference. That's not a disc. That's a muscle doing something it shouldn't be doing.
This matters because the approach to treatment is different depending on what's actually going on. Which is exactly why I do a thorough intake with every new client before we start.
What the Research Says
The science on manual therapy for sciatic-type pain is genuinely encouraging. A review published in Cureus examined physiotherapy techniques for piriformis syndrome and found that approaches including myofascial release, deep friction massage, and nerve mobilization were effective in managing pain and nerve compression symptoms.* The review specifically highlighted that reducing tightness in the piriformis through hands-on work relieves the impingement on the sciatic nerve — which tracks with what I see in practice.
On the broader picture of massage for lower back pain (which often underlies or contributes to sciatic symptoms), a 2023 randomized controlled trial in Medicine found that massage therapy significantly reduced pain intensity, improved sleep quality, and reduced disability scores in patients with chronic mechanical low back pain.** Both connective tissue massage and classical massage produced measurable improvements in pain, autonomic responses, and quality of life after just four weeks of treatment.
And there's more. A 2023 study in the Journal of Sport Rehabilitation found that myofascial release techniques applied to the lumbar region were just as effective at reducing hamstring tightness as working directly on the hamstrings themselves.*** This is fascinating and completely consistent with what I see on the table — the body is connected in ways that aren't always obvious, and loosening up the lumbar fascia and musculature can change what's happening all the way down through the glutes and legs.
That's the kind of whole-body thinking I bring to every session.
How I Work with Sciatica and Sciatic-Type Pain
When someone comes to me for in home massage with sciatica complaints, the first thing I do is listen. I want to know:
Where exactly is the pain? Is it one side or both?
Does it travel? How far?
Does sitting make it worse, or walking?
What's your job? Do you drive a lot?
Any history of disc problems, imaging, or physical therapy?
The answers tell me a lot about where to start looking. Someone who sits at a desk all day and has glute pain that radiates into the back of the thigh? I'm immediately thinking piriformis and hip flexors. Someone with radiating pain that gets worse when they cough or sneeze? That's more suggestive of actual nerve root involvement at the spine, and I'll work accordingly — and refer out to their doctor if needed.
I don't use a menu of services. I approach each session based on what your body actually needs that day. So while the techniques I draw from include deep tissue massage work, myofascial release, sports massage approaches, and targeted stretching — what matters is how those tools get combined for your specific situation.
Here's what working on sciatica and its cousins typically looks like with me:
The glutes and piriformis get the attention they deserve. Most massage therapists spend too much time on the low back and not enough time in the glute complex. The piriformis is deep — it requires sustained, specific pressure to actually reach it. I spend real time here. This is often where the problem lives.
The lumbar region and surrounding fascia. Restrictions in the thoracolumbar fascia (lower back area) can affect everything below. Myofascial release work in this area can shift the tension pattern in ways that allow the whole region to decompress. A 2022 randomized controlled study found that myofascial release techniques to the diaphragm and iliopsoas significantly reduced pain and improved lumbar range of motion in patients with chronic low back pain — improvements in both mobility and pain at rest.**
The psoas and hip flexors. If you've read my post on the psoas, you know this muscle is sneaky. A chronically tight psoas pulls the lumbar spine forward, increases compression on the disc spaces, and throws the whole pelvis out of balance. It's almost always involved when someone has chronic lower back or hip pain. Almost always.
The hamstrings. Tight hamstrings increase the pull on the sit bones, which affects the piriformis, which affects the sciatic nerve. It's all connected. Ignoring the hamstrings when working on sciatica is like fixing a leak without checking the pipes around it.
The gluteus medius — the one everybody forgets. This is the muscle I probably find the most trigger points in, especially with people who sit for a living. The glute med sits on the outer upper portion of the hip, and when it gets loaded up with trigger points it refers pain down the side and back of the hip in a pattern that maps almost perfectly onto what people describe as sciatica. Based on articles retrieved from PubMed, a systematic review in BMC Musculoskeletal Disorders found that people with low back pain consistently showed reduced strength and a higher number of trigger points in the gluteus medius compared to those without pain.**** That finding tracks with what I see on the table constantly. The muscle is underworked, chronically compressed, and completely overlooked by most people (and honestly, a lot of therapists). Spending real time here — sustained pressure, working through the layers — often produces that "how did I not know that was there" reaction that tells me we've found something important.
Why In-Home Massage Is Especially Good for Sciatica
Think about what happens after a great massage when you're dealing with sciatic pain. Your nervous system is calm. Your muscles are loose. The last thing you want to do is put on shoes, walk to a car, sit in traffic on the 405, and drive home.
That's the problem with the spa model for this kind of work. You spend an hour finally getting your body to let go, and then you undo a chunk of it just getting home.
When I come to you — whether you're in Santa Monica, Hollywood, Studio City, or Calabasas — you get to stay horizontal. I set up my table (all I need is about an 8x8 foot space), bring my own sheets, blanket, oil, and music, and when we're done you can lie on the couch, take a bath, or just go to sleep. That's the optimal recovery window, and you get to actually use it.
For a condition like sciatica that is often aggravated by sitting and movement, this isn't just a convenience — it's actually better care.
What to Expect: Realistic Outcomes
I want to be straight with you here, because I think honesty builds trust and also because I've been doing this long enough to know what's realistic.
If your pain is from piriformis syndrome, muscle tension, or fascial restrictions — massage therapy can be genuinely transformative. I've seen people walk out of sessions with significantly less pain than they walked in with, and with a regular maintenance routine, many stay that way.
If you have true disc herniation compressing a nerve root at the spine, massage won't fix the disc. But it can absolutely help manage the surrounding muscle tension, reduce the overall load on the area, and make daily life much more manageable while other interventions (physical therapy, steroid injections, etc.) are also in play. I work alongside a lot of clients who are also seeing chiropractors, orthopedists, or PTs — and there's plenty of room for massage in that picture.
If you're not sure what's going on with your leg pain, it's worth getting evaluated by a physician or orthopedist. I'm not a doctor, and a proper diagnosis matters. But if you've been evaluated and told it's musculoskeletal — or you suspect it is — I'm ready to dig in.
One More Thing: Stop Accepting Leg Pain as Just "Part of Life"
I see this a lot in Los Angeles, especially among people in demanding careers — entertainment, finance, fitness. They've been sitting on sciatic pain (sometimes literally) for months or years, convinced it's something they just have to manage. They've tried stretching, they've tried a heating pad, they’ve sat on a lacrosse ball, they've tried that one YouTube video their trainer sent them…
Sometimes all that helps. But a lot of the time, the underlying issue hasn't actually been addressed. The muscle is still tight. The nerve is still being compressed somewhere along its path. And the body has just adapted to operating in that state, which creates its own set of secondary problems over time.
You don't have to live with that. Whether you're in Bel Air, Marina del Rey, Woodland Hills, or anywhere else I serve across Los Angeles — I come to you, I listen to what's going on, and I get to work on the actual problem.
Ready to start? Book a session here and let's figure out what's really going on with your leg.
References
* Siraj SA, Dadgal R. Physiotherapy for Piriformis Syndrome Using Sciatic Nerve Mobilization and Piriformis Release. Cureus. 2022;14(12):e32952. https://doi.org/10.7759/cureus.32952
** Er G, Yüksel İ. A comparison of the effects of connective tissue massage and classical massage on chronic mechanical low back pain. Medicine (Baltimore). 2023;102(15):e33516. https://doi.org/10.1097/MD.0000000000033516
*** Tamartash H, Bahrpeyma F, Dizaji MM. The effect of remote myofascial release on chronic nonspecific low back pain with hamstrings tightness. Journal of Sport Rehabilitation. 2023;32(5):549–556. https://doi.org/10.1123/jsr.2022-0141
**** Sadler S, Cassidy S, Peterson B, Spink M, Chuter V. Gluteus medius muscle function in people with and without low back pain: a systematic review. BMC Musculoskeletal Disorders. 2019;20(1):463. https://doi.org/10.1186/s12891-019-2833-4